Some of the common nasal problems are:
Headache
Some of the common causes are:
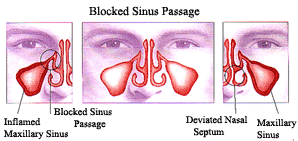
Sinusitis is an inflammation or infection of the lining of one or more air-filled cavities around the nose called the Sinuses. Acute sinusitis results from blocking of the opening of the sinuses following ‘colds’. Mucous collects in the sinuses and can cause discharge and pressure pain in the forehead or face, between the eyes or cheeks depending on which sinuses get involved. If the ‘cold’ lasts longer and the discharge becomes yellow/green, a bacterial infection has taken over giving rise to pain and pressure and occasionally fever. Chronic sinusitis occurs when the sinus opening is blocked for longer period. Headaches are less prominent but congestion and nasal discharge usually persist. Sometimes, fleshy growths called polyps can also develop as a result of exaggerated swelling of the membranes.
A common cold, pharyngitis, allergies, an anatomical abnormality or infrequently an infected tooth can cause sinusitis. Acute sinusitis lasts a short time. Chronic sinusitis lasts longer and is associated with allergies, anatomical abnormalities and repeated acute infections.
Typical complaints include:
Bacterial sinusitis can be treated with antibiotics and medications to relieve symptoms. If left untreated, it can lead to chronic sinusitis, rarely leading to infection of bone around the eyes or meningitis.
Indicators of sinus diseases are nasal obstruction, nasal discharge and sinus headaches. Medical treatment in form of antibiotics, antihistamines, decongestants, may help in eliminating symptoms and disease. If problems persist or are recurrent or are caused by anatomical abnormality, a CT scan is usually performed to elicit more information. If these studies indicate extensive disease surgical treatment in the form of correction of septal deformity, or endoscopic sinus surgery may be required.
Endoscopic sinus surgery is the use of modern technology to treat age-old problems of the nose like sinus blockage. Fibreoptic telescopes with good illumination and magnification enable the ENT. surgeon to visualize directly the blocked nasal passages and sinuses for removing infection, polyps, diseased mucosa to help the sinuses to drain properly, whenever medical therapy has not been successful in alleviating symptoms.
Nasal endoscopy is commonly done for sinusitis, nasal polyps, in cases of bleeding from nose, for diagnosis and follow up of tumours, for sinus headaches. It is also being used for neurosurgical operations like CSF leakage, optic nerve damage and ophthalmic conditions like dacryocystitis.
Nasal endoscopy offers several advantages over earlier treatment modalities
The stay of the patient in hospital is reduced.
The operation is performed by your ENT Surgeon trained in Endoscopic Sinus Surgery. The surgery is performed through the nose with the help of special telescopes called endoscopes which provide excellent visualization. Local anaesthesia or general anaesthesia will be required. It may or may not require hospitalization, (generally one or two days) These procedures are being performed routinely in our centre.
SBleeding is a possibility in any nasal surgery because of numerous blood vessels in the nose. Any extensive sinus surgery runs the risk of cerebrospinal fluid leak or loss of vision. Although these problems are extremely rare with endoscopic sinus surgery, especially in the hands of trained ENT. surgeons.
A ‘sinus headache’ is a headache in the face, forehead, cheeks or around the eyes that comes during a ‘cold’. A vacuum headache can also occur in the sinus areas during descent in an airplane, especially if one has a cold or allergy. Migraine or ‘tension’ headaches can mimic sinus headaches, but they generally go away in a day or two. Sinus headache usually last for days until treated with antibiotics. All headaches that are severe or occur frequently, or prolonged require diagnosis and treatment by a physician.
The inner
Bleeding from the nose is common, unpredictable, and often an inconvenience. The bleeding could occur from either one or both nostrils and may result from a variety of events like sinus infection, trauma, hypertension or tumours.
ear performs two functions, hearing by its cochlear part and maintenance of balance by its vestibular part. Lesions affecting the vestibular part of the ear can cause giddiness, but giddiness can also result from general diseases like high or low blood pressure, diabetes, anaemia and neurological disorders(including tumours). Mental stress can also cause vertigo or aggravate vertigo.
One should always contact the doctor if:
Avoid picking the nose. Avoid blowing the nose for several hours after a nosebleed. Do not strain or bend down to lift anything heavy. Keep head higher than the level of the heart. Use a cotton tipped swab to gently apply petroleum jelly directly on the septum (middle portion of the nose) once or twice a day. Make certain, the fingernails are trimmed to decrease nosepicking. One should always contact the doctor.
Patients of allergic rhinitis complain of nasal blockage, sneezing, watery nasal discharge, loss of sense of smell, headache and post nasal drip.
Medical treatment can be divided into:
Avoidance of allergen: The causative allergen should be identified and whenever possible avoided. This can be done by first taking a detailed history and followed by Skin prick Test. Some of the common allergens include
Drugs: The prime mode of treatment of allergic rhinitis is with the help of drugs.
Topical therapy for long term relief: Local non-surgical treatment for allergic rhinitis in the form of hydrocortisone injections into the inferior turbinate, auto-haemo injections and chemical cautery with 15% silver nitrate (all done once a week for 4-5 times) have been effective in controlling sneezing and rhinorrhoea in large number of patients.
Immunotherapy: specific immunotherapy involves the use of subcutaneous injection of allergen extract in increasing concentrations and decreasing frequency.
Surgical treatment of allergic and vasomotor rhinitis: In patients with allergic rhinitis, the symptoms of nasal obstruction are often compounded due to the presence of anatomical abnormalities including bony and cartilaginous deformities of the septum, hypertrophic turbinates or polyps, which may need surgery.
The noisy sounds of snoring occur when there is an obstruction to the free flow of air through the passages at the back of the mouth and nose. This is the collapsible part of the airway where the tongue and upper throat meet the soft palate and uvula (the fleshy structure that dangles from the roof of the mouth back into the throat). When these structures strike against each other and vibrate during breathing they produce snoring. Persons who snore have at least one of the following problems:
Socially – yes. It is disruptive to family life. It makes the snorer an object of ridicule and causes other household members sleepless nights and resentfulness. Snorers become unwelcome roommates on vacations or business trips. And medically – yes. It disturbs the sleeping patterns of the snorer himself, so that he may not sleep restfully. Furthermore, heavy snorers tend to develop high blood pressure at a younger age than non-snorers. The most exaggerated form of snoring is known as obstructive sleep apnea when loud snoring is interrupted by frequent episodes of totally obstructed breathing.
This is serious if the episodes last over 10 seconds each and occur more than 5 times per hour. During the obstructive episodes, the heart must pump harder to circulate the blood faster. This can cause irregular heartbeats, and after many years it leads to elevated blood pressure and heart enlargement. Persons with obstructive sleep apnea may spend little of their night-time hours in the deep-sleep stages that are essential for a good rest. Therefore, they awaken unrefreshed and are sleepy much of the day. They may fall asleep while driving to work or while on the job.
Adults who are mild or occasional snorers should try the following:
When snoring becomes disruptive to the life of the snorer or his family, medical advice should be sought, especially if other household members suspect the obstructive sleep apnea problem (very loud snoring with periods when all airflow stops – even though the snorer is trying to breathe). The heavy snorer deserves a thorough examination of the nose, mouth, palate, throat, and neck. Studies in a sleep laboratory are valuable to determine how serious the snoring is and what effects it has on the snorer’s health. Treatment will depend, of course, on the diagnosis.
It may be as simple as managing a nasal allergy or infection, surgically correcting a nasal deformity (septoplasty), or removing tonsils and adenoids. Or, snoring/apnea may respond best to surgery on the throat and palate to tighten up flabby tissues and expand the air passages, an operation called UvuloPalatoPharyngoPlasty (UPPP). To the patient it feels like having a tonsillectomy. This can also be performed by Laser Surgery.
If surgery is too risky, unwanted, or unsuccessful, the patient may sleep every night wearing a nasal mask which delivers air pressure into the throat (“CPAP”).
Every chronically snoring child should also be thoroughly examined. Medical evidence suggests a tonsillectomy and adenoidectomy will probably make an important difference in the health and well-being of the child. Snoring means obstructed breathing, and obstruction can be serious.
